 Being in pain can be incredibly debilitating, let alone frustrating. It makes sense to want to get rid of it as fast as possible so your life can return to normal. Many people assume that the quickest way to do this is to get an MRI right away. But as it turns out, that actually slows down your progress!
Being in pain can be incredibly debilitating, let alone frustrating. It makes sense to want to get rid of it as fast as possible so your life can return to normal. Many people assume that the quickest way to do this is to get an MRI right away. But as it turns out, that actually slows down your progress!
This article will discuss when an MRI is warranted and when it’s not and how an MRI can interfere with patient progress. While it is also important to start conservative treatment to speed up healing instead.
What is an MRI?
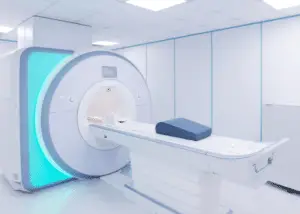 Magnetic Resonance Imaging, or MRI, is a diagnostic tool used to provide images of a person’s anatomy. It provides a picture of the body’s soft tissues and outlines of bones. An MRI is not a necessary acquisition before participating in other forms of care. In fact, studies show that in most cases outcomes can be better in patients that do not have imaging completed before their care. This is especially true for patients with low back pain, which is the most common pain reported.
Magnetic Resonance Imaging, or MRI, is a diagnostic tool used to provide images of a person’s anatomy. It provides a picture of the body’s soft tissues and outlines of bones. An MRI is not a necessary acquisition before participating in other forms of care. In fact, studies show that in most cases outcomes can be better in patients that do not have imaging completed before their care. This is especially true for patients with low back pain, which is the most common pain reported.
Who needs an MRI and Who Doesn’t?
MRIs are appropriate for conditions that display “red flags” such as a history of cancer, fecal or urinary incontinence, accompanying fever, numbness in the groin, and progressive neurological deficits or weaknesses. These are severe symptoms and are rarely seen. In these cases, it is beneficial to secure advanced imaging to rule out cancer relapses, infections, and spinal cord issues.
The vast majority of patients do not need imaging, especially advanced imaging like an MRI. Though they are not pleasant symptoms by any means, radiating pain, numbness and tingling, muscle spasms, and decreases in range of motion are all common to see in patients with low back pain and easily treated by a physical therapist.
Unless a patient is displaying urgent symptoms, like those red flags stated above, they are perfectly able to begin physical therapy. Physical therapy care is a gradual process that will advance with a patient’s abilities and includes consistent re-evaluations to determine the route of the plan of care.
Even if a person without red flags were to get an MRI for a condition like low back pain, their course of care would not be affected, only delayed!
Over 90% of people aged 60 and up that have no back pain at all have “findings” on an MRI. These findings like herniated discs, spinal stenosis, and bulging and degenerated discs, are all normal signs of aging. Just like greying hair and wrinkles on your face, your body changes on the inside too. None of the above findings would be a contraindication for physical therapy.
Unfortunately, back pain symptoms are not well associated with findings on an MRI. Research shows us that even in instances of radiating pain, they still only explain about 30% of cases. Going through the process of obtaining an unnecessary MRI slows down proper care. That delay of care can cause significant detriment to a patient’s potential improvement.
How does an MRI slow down patient progress?
When a person seeks out an MRI before accessing other treatment, it can drastically slow down their ability to heal and recover. Studies have repeatedly shown that it is imperative for patients with low back pain to begin physical therapy care within 14 days of the injury. The earlier the better! When this occurs, the patient is much more likely to recover quickly from their pain. And that’s the goal, isn’t it!

However, when MRI is first sought out, patients lose that quick access to physical therapy while they wait on scheduling their scan and wait longer still to get results back. Likely, those results demonstrate findings that are insignificant, leading to a patient’s wasted time and money.
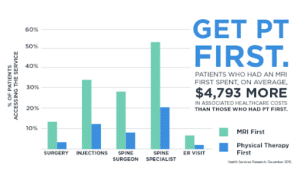
When patients finally do get into physical therapy, those late-comers are using more medical services and thus paying much more for their care.
Aside from breaking the bank, patients that are late to begin physical therapy are also far more likely to be prescribed heavy pain killers and are a staggering 89% more likely to be on the precipice of back surgery.
That’s right, patients that get an MRI are more likely to undergo surgery. This isn’t to say that they are appropriate candidates for surgery though. Those patients typically show no significant improvements a year after their procedure. Unnecessary surgery can lead to complications and increased dysfunction…that’s exactly the opposite of ideal. On top of that, once a person has one lumbar surgery, they’re likely to have multiple.
Let’s compare that to the side effects of physical therapy. There basically are none! Physical therapists are extensively trained to evaluate a patient’s abilities and discern what they can tolerate in a plan of care. Physical therapy is aimed at improving symptoms and function. It is a non-invasive and safe treatment that can greatly benefit nearly any condition.
Conclusion
Unfortunately, MRIs aren’t the golden answer that many people believe them to be. A magnitude of high-quality research studies has shown us that unnecessary MRIs slow down a patient’s access to care, causing them significant longevity of symptoms and much greater health care costs. Take the right step by engaging in physical therapy first, and trust your body’s ability to return to function and come out better and stronger in the end.
Works Referenced:
Mueller K. Wang D. Lea R. The timing of physical therapy for low back pain: does it matter in worker’s compensation? Workers Compensation Research Institute. 2020. https://www.wcrinet.org/reports/the-timing-of-physical-therapy-for-low-back-pain-does-it-matter-in-workers-compensation
Flynn T. Smith B. Chou R. Appropriate use of diagnostic imaging in low back pain: a reminder that unnecessary imaging may do as much harm as good. Journal of Orthopaedic & Sports Physical Therapy. 2011: 41(11): 838-846. https://www.jospt.org/doi/10.2519/jospt.2011.3618
Tousignant-Laflamme Y. Longtime C. Brismee J. How radiological findings can help or hinder patients’ recovery in the rehabilitation management of patients with low back pain: what can clinicians do? Journal of Manual & Manipulative Therapy. 2017; 25(2): 63-65. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5430450/
Other Great Rehab Related Articles
GLP Weight Loss and Back Health: Effective Strategies and Insights
How to Stay Active After Cervical Fractures: Expert Tips and Advice
Dealing with Painful Stairs After Ankle Replacement Surgery
Walking After a Total Ankle Replacement: Tips for a Successful Recovery
Exercises While Non-Weight Bearing After Ankle Replacement: Elevation, AROM, Leg Raises, and More
Ankle Pain with Stairs: Causes and Home Treatment Options
Disclaimer: The information provided in this post is for educational purposes only. This is not a substitute for a medical appointment. Please refer to your physician before starting any exercise program.






