Sustaining a cervical fracture can feel like a major setback, especially when it comes to staying active. It’s essential to focus on safe movements and gradual rehabilitation to regain strength and mobility. Understanding how to stay active after a cervical fracture requires a combination of proper rehabilitation exercises and lifestyle adjustments.
Engaging in light physical activities, such as walking and gentle stretching, is crucial in the early stages of recovery. Over time, incorporating low-impact exercises like swimming or using stationary bikes can help maintain fitness without putting undue stress on the neck. Consulting with physical therapists ensures that exercises are safe and tailored to individual needs.
It’s also important to listen to one’s body and avoid pushing too hard. Monitoring for any pain or discomfort and promptly addressing these issues with healthcare providers helps prevent further injury. Focusing on gradual progress and celebrating small milestones makes staying active both safe and rewarding.
Key Takeaways
- Safe, gradual exercise helps maintain fitness.
- Consultation with physical therapists is crucial.
- Listening to your body prevents further injury.
Understanding Cervical Fractures
Cervical fractures involve the bones in the neck and can vary in severity. They often arise from significant trauma and can lead to serious complications. Understanding the anatomy of the cervical spine, types of fractures, causes, and signs can help in identifying and addressing these injuries effectively.
Anatomy of the Cervical Spine
The cervical spine is composed of seven vertebrae, labeled C1 to C7. These vertebrae support the head and protect the spinal cord, which runs through the spinal column. Ligaments and muscles surrounding the cervical spine provide stability and mobility. The cervical spine has a natural curve, which helps absorb shock and maintain balance.
Vertebrae in the cervical spine are smaller compared to other parts of the spine but are highly flexible. This flexibility is essential for head movement. Nerves branching from the spinal cord exit through openings between the vertebrae, controlling sensations and movements in various parts of the body.
Types of Cervical Fractures
Cervical fractures can be categorized based on the bone structure and nature of the break. The most common types include:
- Compression Fractures: These occur when the vertebra collapses. It’s common in older adults with osteoporosis.
- Burst Fractures: Involves the vertebra breaking into several pieces, often due to high-energy trauma.
- Flexion-Extension Injuries: Result from sudden, forceful movements causing vertebrae to dislocate or fragment.
- Vertebral Fracture: General term for any break in the vertebra.
Each type of fracture has its unique set of challenges and treatment protocols, which can include bracing, physical therapy, or surgery.
Causes and Risk Factors
High-energy impacts such as car accidents or falls are primary causes of cervical fractures. In elderly individuals, even minor falls can lead to fractures due to weakened bones. Athletes involved in contact sports are also at higher risk. Osteoporosis, a condition that weakens bones, increases the likelihood of sustaining a cervical fracture.
Risk factors include:
- Falls, especially from heights
- Automobile accidents
- Sports injuries
- Low bone density due to conditions like osteoporosis
Understanding these causes and risk factors aids in preventive measures and early diagnosis.
Signs and Symptoms
Signs of a cervical fracture can vary but often include:
- Neck pain and tenderness
- Limited range of motion
- Swelling or bruising
- Numbness or tingling in the limbs
In severe cases, there might be visible deformity in the neck region, or complete loss of movement in the affected area. Immediate medical attention is crucial to minimize potential complications, including spinal cord damage.
Identifying signs early and seeking prompt care can significantly enhance recovery outcomes.
Immediate Response to Injury

When dealing with a cervical spine injury, the immediate steps are critical. These include emergency care, imaging for diagnosis, and initial stabilization and management to prevent further damage.
Emergency Care and Assessment
If someone experiences a fall or trauma and shows signs of a cervical spine injury, immediate action is vital. Keep the person still to avoid further injury. Avoid moving their head or neck. Call emergency services immediately.
In the emergency room, medical professionals will assess the patient. They look for signs of spinal cord injury, such as loss of sensation or paralysis. Clinicians often use Advanced Trauma Life Support (ATLS) protocols to guide this assessment.
Physical examinations are crucial. Doctors will check for cervical spine tenderness, deformity, and neurological deficits. It’s essential to identify any life-threatening conditions quickly.
Imaging and Diagnosis
Imaging is necessary to confirm a cervical spine injury. X-rays (plain radiographs) are often the first step. They help rule out fractures or dislocations.
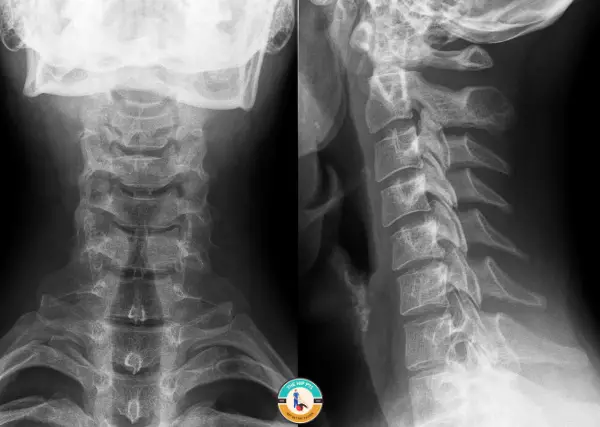
For a more detailed view, healthcare providers may use a CT scan. This imaging technique provides cross-sectional images of the spine. It helps identify subtle fractures that X-rays might miss.
An MRI may also be required. MRIs are particularly useful for visualizing soft tissues, like spinal cord injuries and ligament injuries. This comprehensive imaging helps in planning the appropriate treatment.
Stabilization and Management
Once a cervical spine injury is confirmed, stabilization is crucial. Immobilization devices like collars or braces help keep the spine aligned and prevent further damage.
If the injury is severe, like a fracture-dislocation, immediate intervention might be necessary. Techniques such as traction or surgical stabilization can be used to realign the spine.
Management also involves careful monitoring. Doctors need to watch for complications like swelling or secondary spinal cord injuries. Pain management and physical therapy may be part of the early treatment plan to aid recovery.
Prompt and accurate response to cervical spine injuries can significantly reduce the risk of long-term damage.
Medical and Surgical Treatment Options
Treatment options for cervical fractures often depend on the severity and type of injury. These include conservative approaches and more invasive surgical interventions, with specific care needed after surgery to ensure proper healing.
Conservative Management
For less severe cervical fractures, conservative management is often the first line of treatment. This can include the use of a brace or cervical collar to stabilize the neck and allow ligamentous structures to heal properly. Traction might be used in some cases to align the spine.
Medication for pain relief and muscle relaxation is also typically prescribed. Regular follow-up with physical therapy helps in regaining strength and mobility while keeping the neck stable. The goal here is to avoid invasive procedures by allowing the body to heal itself naturally.
Surgical Interventions
When conservative management is insufficient, surgical interventions may be necessary. Surgery aims to stabilize the spine and protect the spinal cord. Procedures such as odontoid screw placement can be used to directly stabilize fractures.
Other surgeries might involve fusion techniques that use plates, screws, or rods to permanently join vertebrae. The University of Maryland Medical Center states that these surgeries can vary in duration based on complexity. Anterior cervical discectomy and fusion (ACDF) is another common surgery that removes damaged discs to relieve pressure on the spinal cord.
Postoperative Care
Postoperative care is crucial for recovery after cervical spine surgery. Initial care includes managing pain and monitoring for complications like infections or difficulties swallowing, known as dysphagia. These issues can be more common in surgeries utilizing an anterior approach, as highlighted by Spine-Health.
Patients often engage in physical therapy to strengthen neck muscles and regain mobility. Wearing a neck brace may still be necessary to ensure stability as healing progresses. Follow-up appointments are critical to monitor the spine’s alignment and overall recovery process.
Rehabilitation and Recovery
Rehabilitation after cervical fractures focuses on regaining mobility, strength, and reducing muscle spasms. It’s important to participate in physical therapy and monitor progress closely while adopting adaptive techniques to ease daily activities.
Physical Therapy and Exercise
Physical therapy is crucial for recovery. Therapists develop personalized plans that might include gentle neck exercises to help restore range of motion. Patients may also perform low-impact aerobic exercises like walking or swimming to maintain overall fitness without straining the neck.
Stretching exercises are often recommended to reduce muscle tension and spasms. Using resistance bands can help build strength gradually.
Don’t start stretching until you are cleared after follow up imaging that it shows that the fracture is healing.
It’s important to follow the therapist’s guidance to avoid re-injury.
Patients should start with simple activities and slowly increase intensity. Consistency in these exercises can greatly aid recovery.
Monitoring Progress
Tracking progress is essential to ensure the rehabilitation plan is effective. Regular check-ins with healthcare providers can help monitor improvements in mobility and strength.
Pain levels should be documented to adjust the treatment plan as needed. Using tools like a pain journal or mobile app can help keep track of daily symptoms and exercise routines.
Doctors may use imaging tests to check the healing of cervical fractures. These assessments guide decisions on modifying the rehabilitation program. Adjustments should be made according to patient feedback and recovery milestones.
Adaptive Techniques
Living with a cervical fracture requires some adaptations. Using ergonomic tools like special pillows can help maintain proper neck alignment during sleep. Supportive chairs and cushions may also be beneficial during the day.
Patients might need to learn new ways to perform daily tasks to avoid stress on the neck. For example, using tools like reachers or grabbers can help minimize bending and stretching.
Wearing a cervical collar or brace can provide additional support during the early stages of recovery. Occupational therapists can offer valuable advice on adaptive techniques to safeguard against further injury while maintaining independence in daily activities.
Living with a Cervical Fracture
Living with a cervical fracture involves many adjustments to daily life, seeking support, and taking steps to prevent further injury. These changes are essential to maintain mobility, muscle tone, and overall quality of life.
Daily Life Adjustments
Adapting to life with a cervical fracture requires changes in everyday tasks to ensure safety and comfort. Activities like bending, lifting, and even simple movements may need to be modified. Using tools like reachers or long-handled sponges can help minimize strain.
Mobility:
- Use a walker or cane to maintain balance and avoid falls.
- Ensure living spaces are free of clutter and have wide pathways.
Muscle Tone and Sensation:
- Engage in gentle exercises recommended by a physician or physical therapist.
- Pay attention to any changes in sensation or muscle stiffness and report them to a healthcare provider.
Support and Resources
Having the right support can make managing a cervical fracture easier. Seek help from healthcare professionals, community groups, and assistive technology.
Healthcare Providers:
- Physical therapists can design exercise plans to maintain muscle tone and improve mobility.
- Occupational therapists can provide strategies for daily tasks and recommend adaptive equipment.
Community and Online Resources:
- Join support groups for individuals with spinal injuries.
- Utilize online resources and forums for advice and shared experiences.
Assistive Technology:
- Consider devices like cervical collars to reduce neck stiffness and support healing.
- Use voice-activated home assistants to minimize physical strain.
Preventing Further Injury
Preventing additional injuries is critical after a cervical fracture. Precautions should be in place at all times to protect the injured area.
Safety Measures:
- Avoid high-risk activities that may cause falls or sudden impacts.
- Wear a cervical collar as directed by your healthcare provider to limit movement and support healing.
Physical Activity:
- Engage in low-impact exercises, such as swimming or stationary cycling, to improve muscle tone without straining the neck.
- Follow an approved physical therapy regimen to strengthen muscles and enhance sensation.

Home Modifications:
- Install grab bars in bathrooms and along stairways.
- Use non-slip mats and ensure good lighting throughout the home.
By making these adjustments, seeking appropriate support, and taking necessary precautions, individuals can continue to lead active and fulfilling lives even with a cervical fracture.
Understanding Potential Complications
Cervical spine fractures can lead to various complications. These include neurological issues, long-term physical effects, and psychological impacts.
Neurological Implications
Fractures in the cervical spine can damage the spinal cord, resulting in complications such as numbness, tingling, and loss of muscle control. Trauma patients often experience limited range of motion and pain. Cervical spinal cord injuries can cause paralysis below the injury level, sometimes leading to life-threatening conditions. Proper medical evaluation and treatment are critical to prevent severe outcomes.
Long-Term Physical Effects
Persistent pain and reduced mobility are common long-term effects. Muscle weakness and atrophy can occur even after the fracture has healed. Patients might experience chronic pain due to nerve damage and other complications.
Another concern is the increased risk of infection, which can further impair recovery. Regular physical therapy helps manage these physical effects and improve quality of life.
Psychological Considerations
Cervical spine fractures can affect mental health. Patients might experience anxiety, depression, and fear related to their injury and recovery process. Dealing with long-term pain and physical limitations can worsen these psychological issues. Emotional support, counseling, and therapy are essential to address these concerns. Recognizing and managing psychological impacts is vital for comprehensive recovery.
Special Considerations
When staying active after cervical fractures, there are unique needs for different groups such as pediatric and elderly patients, athletes, and those requiring occupational therapy. Each group faces specific challenges and benefits from tailored care and activities.
Pediatric and Elderly Patients
Pediatric and elderly patients need special attention due to their unique physiology. Elderly patients often have conditions such as osteoporosis, which makes their bones more fragile. They are also at a higher risk of falling, which can complicate recovery. Physical therapists may recommend gentle activities like walking or swimming to maintain mobility without putting too much strain on the spine.
Pediatric patients heal more quickly generally but require careful monitoring to avoid reinjury. Activities need to be safe and adjusted to their growth patterns. Exercises like yoga can help improve flexibility and strength while keeping the young patient engaged.
Athletes Returning to Sport
For athletes, returning to their sport after a cervical fracture is a critical process. They need to rebuild strength and flexibility while avoiding further injury. A comprehensive rehab program tailored to their specific sport is essential. This program might include:
- Strength training: Focus on neck muscles to protect the cervical spine.
- Flexibility exercises: Stretching routines to maintain a range of motion.
- Sport-specific drills: Gradual reintroduction of sport activities to ensure readiness.
Monitoring for back pain and swelling is vital. Coaches and medical staff should work together to create a safe return-to-play schedule.
Occupational Therapy
Occupational therapy plays a key role in helping patients regain everyday functionality after a cervical fracture. Therapists focus on improving daily living activities like dressing, eating, and bathing through adaptive techniques.
- Custom exercises: To strengthen muscles and maintain back stability.
- Tools and gadgets: Can help with tasks that might be challenging after a fracture.
- Alcohol and medication management: Educate patients on avoiding substances that could interfere with healing or increase fall risk.
Therapists work closely with patients to set realistic goals and monitor their progress, which helps in maintaining motivation and ensuring a steady recovery.
Collaborative Care Approach
A collaborative care approach ensures that patients recover well from cervical fractures. It involves the support of healthcare professionals, family members, and community resources working together.
Role of Interprofessional Team
An interprofessional team is essential for effective recovery from cervical fractures. The team includes doctors, nurses, physical therapists, and occupational therapists. Doctors focus on medical treatments and monitoring the patient’s progress.
Nurses provide day-to-day care and manage medications. Physical therapists design exercise programs to regain strength and mobility, while occupational therapists help patients relearn daily activities. This team approach ensures that all aspects of the patient’s health are addressed, allowing for a coordinated and comprehensive recovery plan. Regular communication among team members is vital to adapt care plans based on the patient’s progress and needs.
Family and Caregiver Support
Family and caregiver support plays a crucial role in the recovery process. They help with daily activities, such as bathing, dressing, and meal preparation. Emotional support from family members can boost the patient’s morale and motivation to stick with rehabilitation exercises.
Caregivers also assist in transportation to and from medical appointments and ensure that the patient follows medical advice and therapy routines. Educating family members and caregivers about the patient’s specific needs helps in providing better care. They act as a critical link between the patient and the healthcare team, ensuring that any changes in the patient’s condition are promptly addressed.
Community Resources
Community resources can offer additional support for those recovering from cervical fractures. Local support groups provide emotional support and share practical advice for managing daily challenges. Rehabilitation centers offer specialized programs to improve mobility and independence.
Home care services can supply medical equipment such as wheelchairs or neck braces. Non-profit organizations may provide financial aid for medical expenses or transportation. Local health departments often run programs to educate patients and families about long-term care strategies. Leveraging these resources helps create a supportive environment that facilitates recovery and improves quality of life.
Frequently Asked Questions
Recovery from a cervical fracture requires specific exercises, avoidance of certain activities, and adherence to specific guidelines. Here are answers to some common questions about staying active after a cervical fracture.
What are the recovery exercises recommended after a cervical spine injury?
Physical therapy exercises often include gentle neck stretches and strengthening activities. Exercises such as chin tucks, shoulder blade squeezes, and gentle neck rotations are usually recommended. Always follow a physical therapist’s guidance.
Are there specific activities that should be avoided following a compression fracture?
Yes, heavy lifting, high-impact sports, and activities that strain the neck should be avoided. It’s important to steer clear of activities that risk further injury until a healthcare provider gives the all-clear.
How long is the typical healing process for a cervical fracture?
The healing process can vary greatly, but it generally takes about 6 to 12 weeks. Factors like the severity of the fracture and adherence to medical advice can influence recovery time.
What is the safe approach to physical activity post-cervical fusion surgery?
After cervical fusion surgery, engaging in low-impact activities is crucial. Walking and stationary cycling are often recommended. Avoid high-impact sports and heavy lifting to ensure proper healing.
Can you improve your life expectancy with specific exercises after a compression fracture?
While specific exercises can improve mobility and strength, ensuring a healthy lifestyle overall is more likely to impact life expectancy. Consistent physical activity along with proper nutrition can contribute to better long-term health.
What guidelines should be followed when returning to sports after a cervical spine injury?
Gradual reintroduction to sports is essential. Start with low-impact activities and slowly increase intensity. Always use proper protective gear and seek clearance from a healthcare professional before fully resuming sports activities.
Conclusion
Staying active after a cervical fracture is essential for recovery and long-term health. Follow doctor’s advice and work with medical professionals.
It’s crucial to start with gentle exercises, like neck stretches and light aerobic activities. This can help maintain range of motion and prevent stiffness.
Patients often benefit from physical therapy. Therapists create personalized plans focusing on strength and flexibility, tailored to each individual’s needs.
Key Points to Remember:
- Start Slow: Begin with light exercises to avoid further injury.
- Consistency: Regular activity is better than sporadic, intense sessions.
- Professional Guidance: Always follow a medical professional’s recommendations.
Using supportive devices such as cervical collars can aid stability. This allows safer movement during the initial stages of recovery.
Emotional well-being is important too. Remaining active can improve mood and mental health, which can be challenging after an injury.
Helpful Tips:
- Set realistic goals.
- Monitor progress.
- Stay positive and patient.
Engaging in low-impact sports like swimming or walking helps maintain an active lifestyle without putting too much strain on the neck.
Incorporating these strategies can aid in a smoother, more effective recovery, ensuring that individuals remain active and healthy.
Disclaimer: The information provided in this post is for educational purposes only. This is not a substitute for a medical appointment. Please refer to your physician before starting any exercise program.
