The human hip joint is the foundation of the core, the base of stability, and an integral axis for force and strength. With great power, however, comes the possibility of great dysfunction. Hip pain is one of the most common complaints among patients seeking assistance from a Physical Therapist. Difficulties with daily activities such as walking, using stairs, laying on the painful side are all common symptoms of a condition affecting the outside of the hip known as Greater Trochanteric Pain Syndrome, or GTPS.
Pain involving the lateral hip is a very prevalent issue, affecting up to 25% of the general population.
In the past, patients with these symptoms were frequently diagnosed with “trochanteric bursitis”. However, the distinguishing features of inflammation and radiological findings of bursitis are not seen in all patients with lateral hip pain. More often in these patients, tendinopathy is the significant discovery on imaging – though, bursitis and tendinopathy can often coexist. Therefore, the preferred term to describe conditions involving lateral hip pain is Greater Trochanteric Pain Syndrome. Conservative interventions are the ideal form of treatment and Physical Therapy is known to resolve nearly all cases of GTPS.
What is Hip Bursitis?
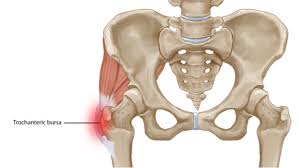
Due to the complexity and intricacies of the hip joint structure, it is very susceptible to the effects of muscular imbalances and overuse. Crossing the hip are the tendons of the hip flexor, quad, and gluteal muscles. There are multiple bursae, fluid filled sacs, dispersed throughout and in between tendons and bones for the purpose of decreasing friction. Though the cause of GTPS is known to be tendinopathy, at times this inflammation and degeneration of the tendons can also accompany irritation of a bursa. This bursitis is a secondary concern next to the origin of the condition.
What are the Causes of Bursitis?
Through overuse or chronic deconditioning and weakness, excess strain is placed upon the gluteal muscles that aid in stabilizing the hip. This leads to a degeneration of the tendons themselves, resulting in symptoms of pain. The population that most tends to exhibit this weakness and it’s resulting pain syndrome are women between 40-60 years of age. Overweight patients and long distance runners are also at risk for GTPS due to increased stress on the hip joint. Those with leg length discrepancies or chronic low back pain are susceptible for the same reason.
What are the Symptoms of Hip Bursitis?
The characteristic symptoms of GTPS are pain on the outside of the hip and acute tenderness right on top of the hip bone. Coordinating symptoms can include radiating pain and difficulties with certain activities. Localized swelling and redness is not typically associated with GTPS.
Common symptoms include:
- Pain traversing stairs
- Pain lying on the side at night
- Tenderness on the outside of the hip
- Pain on the outside of the hip radiating to the outer knee or buttocks
- Pain with running and sports activities
- Difficulty getting up from sitting down
- The feeling of joint stiffness in the hip
Treatment Options for Hip Bursitis and Glute Tendinopathy
The preferred method of treating GTPS is through a combination of activity modification and exercise therapy. Initial treatment of rest, ice, and activity modification is key. Following this phase, a progression into correcting muscular imbalances should be implemented.
Corticosteroid injections are sometimes used, though symptom recurrence is very likely and long term weakening of the tendon structure is a possible side effect. Multiple studies have demonstrated that injections do not result in significant lasting results. Exercise therapy is much more effective in providing long term and consistent relief.
The Best Exercises for Hip Bursitis and Lateral Hip Pain
Soft Tissue Massage
Place a dense ball (like a lacrosse ball) or foam roller, between a wall and the outside of your hip. Gently rock your hips side to side and up and down to roll the ball along your sore muscles. Vary the pressure against your hip by leaning more into the ball. This can also be performed on the back of the hip.
Hip Extension
Lay on your stomach on the ground. Tighten your core and slowly lift one leg off of the ground. You should feel your glute muscles working here. Try to keep your hips even on the ground, and avoid rolling to the side. Hold for a few seconds, then slowly lower. Repeat on the other side. Progress this exercise by adding a light ankle weight.
Plank
Lay on your stomach on the ground, and prop up onto your forearms and place your toes on the ground. With an inhale, lift your body up off the ground into a plank position. Keep your shoulders, hips, and knees aligned. Hold for 30 seconds (or longer), then slowly lower down to rest. Repeat for 5 iterations. Progress this exercise by lifting up from your hands into a full push up position.
Side Plank
Lay on your side (use a cushion under your hip if this is uncomfortable) with your body in a straight line from shoulders to ankles. Prop up onto your bottom forearm and the outside of your bottom foot. With an exhale, lift your hips up off the ground from your forearm and foot, into a side plank. Hold for 20 seconds (or longer), then slowly lower back down with control. Perform 5 iterations on each side. Progress this exercise by lifting up from your hand, instead of your forearm.
Monster Walk
Place a light resistance band around your knees. Keeping your toes pointed forward, begin side stepping in slow small steps – enough to feel the resistance and avoid slack in the band. Perform 10-15 steps in one direction, then step in the opposite direction. To progress this exercise, move the band to your ankles.
Other Tips to Reduce Pain With Hip Bursitis
Outside of exercises and stretches, there are some other modifications you can do to decrease your hip pain. Some of these include;
- Sleeping with a knee pillow for comfort
- Try going up and down stairs with the same lead foot until your hip feels better
- Try low weight-bearing exercise such as swimming for bilking
- Reduce overall obesity and weight gain to decrease strain through your hips
FAQ for Hip Bursitis
What Position Should I Sleep in for Hip Bursitis?
For the most part, sleeping on your side will be the most comfortable position to sleep in. You may not be able so to sleep on the involved side however, sleeping on the good side with a knee pillow is usually the most comfortable.
Should I Foam Roll Hip Bursitis

Does Kinesiotape Work for Hip Bursitis?
Kinesiotape is a good and safe way to try and minimize hip pain with bursitis. It adds a simple level of support and can take some of the pressure off the bursa and tendon. Our favorite type of kinesiotape is Rock Tape.
Can I Run With Hip Bursitis?
We tend to recommend against running when someone is experiencing hip bursitis as the loads on the hip muscles are often too high and cause quite a bit of discomfort with running. Once you have recovered and no longer symptomatic, feel free to work back to your normal running levels.
Key Take Aways
A debilitating and complicated condition, Greater Trochanteric Pain Syndrome is a result of a combination of weakness, imbalances, and overuse. A controlled progression through a customized rehabilitation protocol is key to overcoming these challenges. Patience, perseverance, and the guidance of your Physical Therapist can ensure that you successfully conquer your symptoms.
Works Referenced:
Speers CJB, Bhogal GS. Greater trochanteric pain syndrome. British Journal of General Practice. 2017; 67: 479-480. https://bjgp.org/content/bjgp/67/663/479.full.pdf
Reid D. The management of greater trochanteric pain syndrome: a systematic literature review. The Journal of Orthopedics. 2016; 16: 15-28. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4761624/pdf/main.pdf
Canoso JJ, Isaac Z, Curtis MR. Greater trochanteric pain syndrome (formerly trochanteric bursitis).
Brinks A, et al. Corticosteroid Injections for Greater Trochanteric Pain Syndrome: A Randomized Controlled Trial in Primary Care. The Annals of Family Medicine. 2011; 9(3)
Bouno AD, Papaila R, Khanduja V, Denaro V, Maffuli N. Management of the greater trochanteric pain syndrome: a systematic review. British Medical Bulletin. 2012; 102: 115-1311. https://www.researchgate.net/profile/Nicola_Maffulli/publication/51619834_Management_of_the_greater_trochanteric_pain_syndrome_A_systematic_review/links/02e7e530b77f386fb0000000/Management-of-the-greater-trochanteric-pain-syndrome-A-systematic-review.pdf
Disclaimer: The information provided in this post is for educational purposes only. This is not a substitute for a medical appointment. Please refer to your physician before starting any exercise program.



